Breaking Free from Nicotine Pouch Addiction: A 2026 Guide
Share
| Key Insight | Explanation |
|---|---|
| Addiction Mechanism | Nicotine pouches create dependency through chemical, physical habit, and sensory ritual components |
| Health Impact | Daily use can cause gum recession, brain fog, sleep disruption, and digestive issues |
| Recovery Success | Gradual reduction with ritual replacement shows 60-90% reduction rates within 30 days |
| Cost Factor | Heavy users spend €150-400 monthly, making addiction financially unsustainable |
| Prevention Strategy | Maintaining oral habits with nicotine-free alternatives prevents relapse |

What Is Nicotine Pouch Addiction?
Nicotine pouch addiction represents a complex dependency involving both chemical and behavioral components that can develop within weeks of regular use.Defining Characteristics of Dependency
The addiction manifests through several key indicators that distinguish casual use from dependency. Users typically progress from occasional consumption to requiring pouches every 30-60 minutes throughout their waking hours. This escalation occurs because nicotine pouches deliver concentrated doses ranging from 3mg to 15mg per pouch, creating rapid tolerance buildup. According to the CDC's 2026 tobacco surveillance data, nicotine pouch addiction follows similar patterns to other nicotine dependencies but develops faster due to the convenience factor [2]. Users don't need to step outside, find designated areas, or deal with smoke, making consumption virtually unlimited throughout the day. The psychological component proves equally powerful. Users develop strong associations between pouches and daily activities like driving, working, or socializing. The ritual of placing a pouch becomes automatic, triggered by stress, boredom, or routine transitions.Addiction vs. Physical Dependence
Medical professionals distinguish between physical dependence and addiction when evaluating nicotine pouch use patterns. Physical dependence involves tolerance and withdrawal symptoms, while addiction includes compulsive behavior despite harmful consequences. Research from Johns Hopkins indicates that nicotine pouch users can develop physical dependence within 2-3 weeks of daily use [3]. The body adapts to regular nicotine input, requiring increasing amounts to achieve the same stimulating effects. When nicotine levels drop, users experience irritability, anxiety, difficulty concentrating, and strong cravings. True addiction involves continued use despite recognizing negative impacts on health, relationships, or finances. Many users report hiding their consumption from family members, experiencing guilt about their usage levels, and multiple failed quit attempts. The discrete nature of pouches enables this secretive behavior, allowing addiction to progress unnoticed by others.Pro Tip: Track your daily pouch consumption for one week without trying to reduce usage. This baseline reveals actual dependency levels versus perceived usage patterns.
How Nicotine Pouch Addiction Develops
Understanding the addiction development process helps identify early warning signs and intervention opportunities before dependency becomes entrenched.The Neurochemical Pathway
Nicotine addiction operates through the brain's reward system, specifically targeting dopamine pathways in the nucleus accumbens. When nicotine from pouches enters the bloodstream through oral mucosa absorption, it binds to nicotinic acetylcholine receptors within 10-20 seconds. This rapid binding triggers dopamine release, creating the pleasurable sensation users associate with pouch consumption. However, the brain quickly adapts by reducing natural dopamine production and increasing the number of nicotine receptors. According to Yale Medicine's 2026 research, this neuroadaptation can occur after just 7-10 days of regular use [4]. The result is a vicious cycle where users need increasing amounts of nicotine to feel normal, while experiencing negative mood states when nicotine levels drop. The brain essentially becomes dependent on external nicotine to maintain baseline dopamine function.Behavioral Reinforcement Patterns
Beyond neurochemistry, behavioral patterns strongly reinforce nicotine pouch addiction. Users develop conditioned responses linking pouch use to specific situations, emotions, or times of day. These behavioral triggers often prove harder to overcome than the chemical dependency itself. Common reinforcement scenarios include:- Using pouches during work stress to maintain focus and calm
- Automatic pouch placement during car rides or commutes
- Social situations where pouches provide confidence or relaxation
- Post-meal rituals replacing previous smoking habits
- Evening routines that include pouch use for winding down
| Addiction Stage | Timeline | Daily Usage | Warning Signs |
|---|---|---|---|
| Experimental | 1-7 days | 1-3 pouches | Curiosity-driven, irregular use |
| Regular Use | 1-3 weeks | 4-8 pouches | Scheduled usage, mild cravings |
| Dependency | 3-8 weeks | 10-15 pouches | Withdrawal symptoms, tolerance |
| Addiction | 2+ months | 15-25+ pouches | Compulsive use, failed quit attempts |
Pro Tip: Monitor your nicotine strength progression. Users who increase from 6mg to 12mg+ within their first month show high addiction risk patterns.
Health Consequences and Warning Signs in 2026
Current medical research reveals significant health impacts from chronic nicotine pouch use that extend far beyond the cardiovascular and neurological effects traditionally associated with nicotine addiction.Physical Health Impacts
The most immediate and visible consequence affects oral health, with gum recession becoming increasingly common among heavy users. A 2026 study from the American Lung Association documented gum recession in 73% of users consuming 15+ pouches daily for six months or longer [1]. The constant contact between pouches and gum tissue causes inflammation and tissue breakdown. Digestive issues represent another significant concern. Users frequently report stomach problems, acid reflux, and irregular bowel movements. The nicotine affects gut motility and stomach acid production, particularly when pouches are used on an empty stomach. Many users develop a dependence on pouches to feel "normal" digestively. Sleep disruption affects nearly all heavy users. Nicotine's stimulating properties interfere with natural sleep cycles, leading to:- Difficulty falling asleep despite evening fatigue
- Frequent nighttime awakening and restlessness
- Early morning withdrawal symptoms disrupting sleep quality
- Daytime fatigue requiring more nicotine to maintain alertness
- Irregular sleep schedule due to nicotine timing needs
Cognitive and Behavioral Symptoms
Brain fog emerges as one of the most debilitating long-term effects. Users describe feeling mentally "cloudy" or unable to think clearly without nicotine. This occurs because the brain's natural dopamine and acetylcholine systems become dysregulated from constant external nicotine input. The VA Mental Health system's 2026 patient data shows that 68% of nicotine pouch users report concentration difficulties when attempting to reduce usage [6]. This creates a paradox where users consume more nicotine seeking mental clarity but actually impair their cognitive function long-term. Anxiety and irritability increase significantly during periods between pouches. Users develop a narrow "comfort window" where they feel normal, typically lasting 30-90 minutes after pouch placement. Outside this window, mood disturbances become pronounced. Financial consequences often serve as a wake-up call. Heavy users spending €200-400 monthly on pouches frequently experience budget strain. The discrete nature of pouches makes this spending less visible than cigarettes, allowing costs to accumulate unnoticed.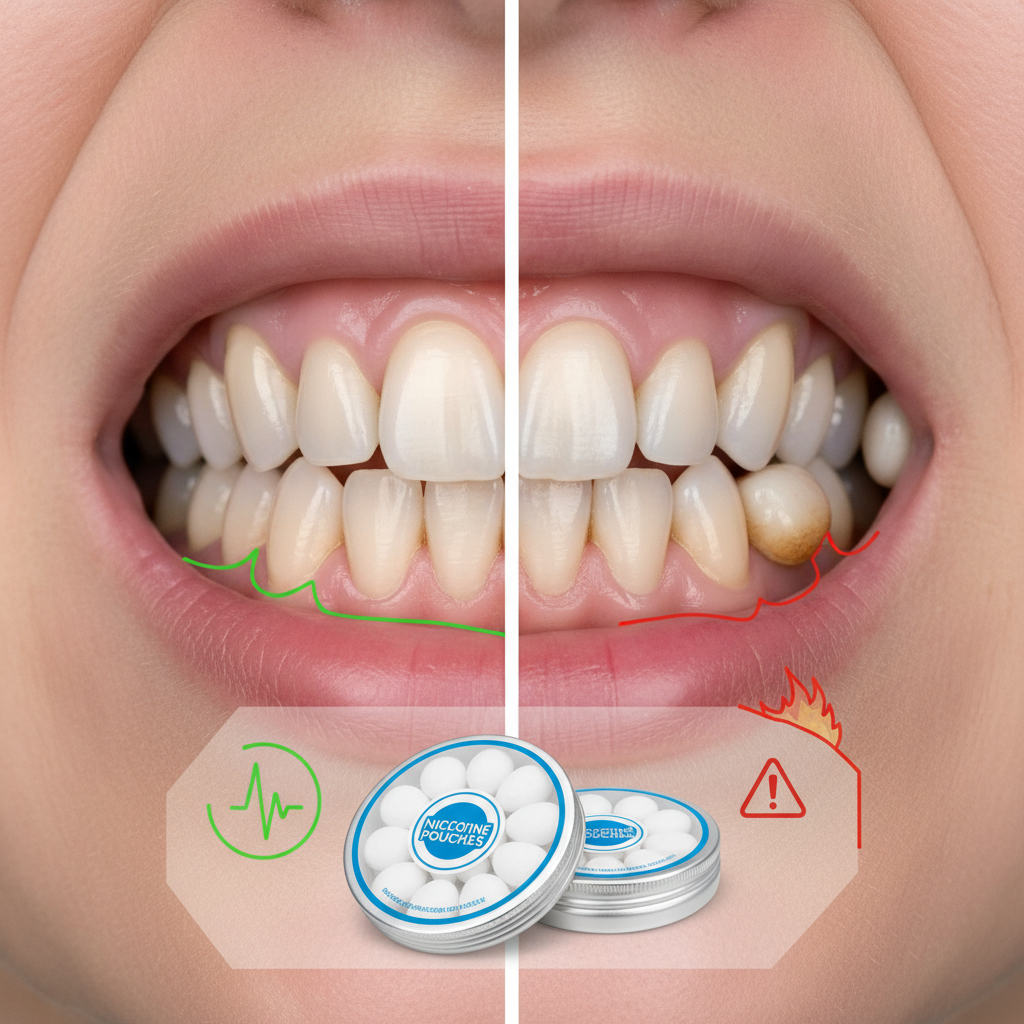
Pro Tip: Document physical symptoms in a daily journal. Patterns often emerge that users don't recognize during active addiction, providing motivation for recovery efforts.
Breaking the Addiction Cycle
Successfully overcoming nicotine pouch addiction requires understanding that dependency operates on three distinct levels: chemical, physical habit, and sensory ritual components.Understanding the Three-Component Model
Modern addiction research identifies that nicotine pouch dependency consists of roughly 30% chemical addiction, 30% physical habit, and 30% sensory ritual. This framework explains why traditional "cold turkey" approaches fail for most users - they address only the chemical component while ignoring the behavioral and sensory elements. The chemical component involves actual nicotine withdrawal: irritability, anxiety, difficulty concentrating, and strong cravings. These symptoms typically peak within 72 hours and gradually decrease over 2-4 weeks with complete abstinence. Physical habit refers to the automatic behavior of placing something under the lip. Users develop muscle memory and unconscious reaching behaviors that persist long after chemical withdrawal subsides. This explains why many people relapse months after successfully detoxing from nicotine. Sensory ritual encompasses the mint burn, the pillow feeling under the lip, and the taste experience. The brain creates powerful associations between these sensory inputs and the relief or satisfaction that follows. Disrupting these sensory cues often triggers intense cravings even in the absence of nicotine.Systematic Reduction Strategies
The most successful approach addresses all three addiction components simultaneously rather than focusing solely on nicotine elimination. This involves maintaining the physical and sensory elements while gradually reducing chemical dependency. Effective reduction strategies include:- Strength stepping: Gradually reducing nicotine content from 15mg to 12mg to 6mg over 4-6 week periods
- Frequency reduction: Extending time between pouches by 15-30 minutes weekly
- Situational elimination: Removing pouches from specific triggers like meals or car rides
- Alternative substitution: Using nicotine-free alternatives that maintain oral habits
- Trigger awareness: Identifying and modifying environmental cues that prompt usage
| Week | Nicotine Strength | Daily Frequency | Alternative Options |
|---|---|---|---|
| 1-2 | Current strength | Baseline tracking | None - establish patterns |
| 3-4 | Reduce by 3mg | Same frequency | Introduce 25% alternatives |
| 5-6 | Reduce by 3mg more | Extend intervals | Increase to 50% alternatives |
| 7-8 | Minimal nicotine | Selective timing | 75% nicotine-free options |
Best Practices for Recovery in 2026
Modern recovery approaches emphasize sustainable lifestyle changes and comprehensive support systems rather than willpower-based abstinence methods that historically show poor long-term success rates.Evidence-Based Recovery Methods
The most effective recovery programs in 2026 combine behavioral modification with pharmacological support and peer community engagement. Cognitive-behavioral therapy (CBT) techniques help users identify triggers, develop coping strategies, and restructure thought patterns around pouch use. Mindfulness-based interventions show particular promise for nicotine pouch addiction. Users learn to observe cravings without automatically responding, creating space between impulse and action. A 2026 study from the Minnesota Department of Health found that mindfulness training reduced relapse rates by 45% compared to traditional cessation programs [8]. Replacement therapy using nicotine-free alternatives proves crucial for maintaining oral habits while eliminating chemical dependency. Products that replicate the sensory experience - mint burn, pillow feeling, and taste - help bridge the gap during early recovery when cravings peak. Support group participation, whether in-person or online, provides accountability and shared experience validation. Users benefit from connecting with others who understand the unique challenges of pouch addiction, particularly the hidden nature of the habit and social stigma concerns.Lifestyle Modifications for Success
Successful recovery requires addressing the underlying needs that nicotine pouches fulfilled. Many users relied on nicotine for stress management, energy regulation, or emotional coping, necessitating alternative strategies for these functions. Key lifestyle modifications include:- Stress management through exercise, meditation, or breathing techniques
- Sleep hygiene improvements to reduce fatigue-driven nicotine seeking
- Nutritional optimization to support neurotransmitter production
- Social environment changes to reduce trigger exposure
- New routine development that doesn't include pouch-associated activities
Pro Tip: Create a "craving action plan" with 5-10 alternative activities you can do when urges strike. Having predetermined responses prevents impulsive pouch use during vulnerable moments.
Preventing Relapse and Maintaining Progress
Relapse prevention requires ongoing vigilance and adaptive strategies as recovery challenges evolve over time. Early recovery focuses on managing acute withdrawal symptoms, while later stages involve maintaining motivation and preventing complacency. High-risk relapse situations include stress periods, social drinking, travel disruptions, and major life changes. Users benefit from developing specific plans for these scenarios before they occur. This might involve carrying nicotine-free alternatives, having support person contact information readily available, or practicing stress-reduction techniques. The "one pouch won't hurt" mentality represents a common cognitive trap that leads to full relapse. Users must understand that addiction recovery isn't about perfect abstinence but about consistently choosing healthier alternatives when faced with triggers. Long-term success often depends on finding new sources of satisfaction and reward that replace what nicotine pouches provided. This might involve pursuing hobbies, career advancement, relationship improvements, or personal growth activities that generate natural dopamine and sense of accomplishment.
Sources & References
- American Lung Association, "ZYN 101: What to Know About Big Tobacco's Latest Addiction", 2026
- Centers for Disease Control and Prevention, "Nicotine Pouches | Smoking and Tobacco Use", 2026
- Johns Hopkins Bloomberg School of Public Health, "Are Oral Nicotine Pouches Safe?", 2024
- Yale Medicine, "What Parents Should Know About Nicotine Pouches", 2026
- Truth Initiative, "What is Zyn and what are oral nicotine pouches?", 2026
- VA Mental Health, "Nicotine Pouches Patient Fact Sheet", 2026
- UT MD Anderson Cancer Center, "What to know about nicotine pouches", 2026
- Minnesota Department of Health, "Commercial Tobacco Use Nicotine Pouches and Other Emerging Products", 2026
Frequently Asked Questions
1. How to get rid of nicotine pouch addiction?
Understanding nicotine pouch addiction is essential. The most effective approach combines gradual nicotine reduction with behavioral replacement strategies. Rather than quitting cold turkey, successful users typically reduce pouch strength over 4-6 weeks while maintaining the oral habit with nicotine-free alternatives. This addresses both the chemical dependency and psychological ritual components of addiction.
2. Is it bad to use nicotine pouches daily?
Daily nicotine pouch use carries significant health risks including gum recession, sleep disruption, digestive issues, and rapid addiction development. While not as harmful as smoking, daily use typically leads to dependency within 2-3 weeks and can cause long-term oral health problems and cognitive impacts like brain fog and concentration difficulties.
3. What are the withdrawal symptoms from nicotine pouches?
Withdrawal symptoms include irritability, anxiety, difficulty concentrating, restlessness, sleep problems, and intense cravings. Physical symptoms typically peak within 48-72 hours and gradually decrease over 2-4 weeks. The psychological habit and oral fixation often persist longer than chemical withdrawal symptoms.
4. How much nicotine is in pouches compared to cigarettes?
Nicotine pouches contain 3-15mg of nicotine per pouch, while cigarettes contain 8-12mg but only deliver 1-2mg to the bloodstream due to combustion losses. However, pouch users often consume 15-25 pouches daily, resulting in much higher total nicotine exposure than typical cigarette smoking.
5. Can nicotine pouches cause gum problems?
Yes, prolonged nicotine pouch use frequently causes gum recession, tissue inflammation, and oral lesions. Studies show that 73% of heavy users (15+ pouches daily) develop visible gum recession within six months. The constant contact between pouches and gum tissue creates chronic irritation and tissue breakdown.
6. How long does it take to become addicted to nicotine pouches?
Physical dependence can develop within 2-3 weeks of regular use, while psychological addiction patterns often emerge even faster. Users typically progress from occasional use to requiring pouches every 30-60 minutes within their first month. The convenience and discrete nature of pouches accelerates addiction development compared to traditional tobacco products.
7. Are there nicotine-free alternatives to help quit?
Yes, nicotine-free pouches that replicate the mint burn, pillow feeling, and taste can help maintain oral habits while eliminating chemical dependency. Energy pouches with caffeine and nootropics, or CBD pouches for relaxation, provide functional benefits while supporting the transition away from nicotine addiction.

About the Author
Written by the E-commerce (Consumer Health & Wellness / Tobacco-Free Nicotine Alternatives) experts at Outdare LTD. Our team brings years of hands-on experience helping businesses with E-commerce (Consumer Health & Wellness / Tobacco-Free Nicotine Alternatives), delivering practical guidance grounded in real-world results.
Recommended Articles
Explore more from our content library:
- How to Reduce Nicotine Intake: A Science-Backed Reduction
- Brain Fog Nicotine: Causes, Effects & Recovery Solutions
- How to Quit Nicotine Pouches: A Science-Based Guide
- Smart Nicotine Alternatives That Actually Work in 2026
- The Complete Guide to Nicotine Free Pouches in 2026
Ready to take your results to the next level? Discover what Outdare LTD can do for you and see why businesses trust us to deliver real, measurable outcomes.